INTERVENTIONAL CARDIOLOGY ASSESSMENT
About INTERVENTIONAL CARDIOLOGY ASSESSMENT
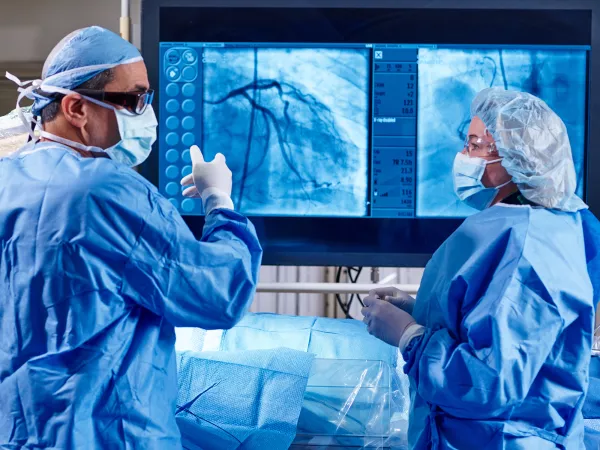
Minimally invasive solutions for healthier hearts
Interventional cardiology assessment identifies children who can benefit from minimally invasive catheter-based procedures instead of open-heart surgery. These procedures include device closure of defects such as ASD, VSD, and PDA, balloon valvotomy for narrowed valves, and stenting for vessel obstruction. Our assessment evaluates anatomy, symptoms, and test findings to ensure safety and suitability.
This approach reduces pain, avoids large scars, shortens hospital stay, and ensures quicker recovery. Families receive clear explanations, expected outcomes, and preparation guidance. Post-procedure follow-up ensures the heart heals well and normal activities resume safely.
Step by Step Process
A structured evaluation to determine suitability for catheter-based procedures, ensuring accurate diagnosis,
safety planning, and smooth recovery for minimally invasive cardiac treatments.
Initial Consultation
Symptoms, history, and prior reports are reviewed to understand heart condition severity, determine concerns, and evaluate potential suitability for catheter-based intervention.
Diagnostic Testing
Echocardiography, ECG, and additional imaging assess anatomy, blood flow patterns, defect size, and valve function for deciding possible interventional treatment options safely.
Risk Assessment
Cardiologist evaluates procedural risks based on age, defect characteristics, vessel size, and associated conditions, ensuring best outcomes with minimal complications expected.
Family Counseling
Parents receive detailed explanation of procedure steps, benefits, risks, anesthesia requirements, recovery expectations, and follow-up needs for informed decision-making.
Interventional Procedure
Catheter is inserted through a vein or artery, guided to the heart, correcting defects using balloons, stents, or closure devices safely for improved long-term outcomes.
Post-Procedure Monitoring
Vitals, rhythm, oxygenation, and healing are monitored; medications are prescribed; follow-up visits scheduled to confirm successful correction and support recovery progress.
Symptoms of Interventional cardiology assessment
Spotting signs needing minimally invasive intervention
Symptoms suggesting interventional treatment include persistent murmurs, rapid breathing, poor feeding, recurrent infections, easy fatigue, poor growth, fainting episodes, or exercise intolerance. Children with ASD, VSD, PDA, valve narrowing, or vessel obstruction may show subtle signs like sweating while feeding, irritability, or frequent hospital visits. These symptoms can indicate heart defects that benefit from catheter-based solutions. Early recognition ensures timely assessment, prevents complications, and avoids progression to more severe disease requiring surgery.

Treatments of Interventional cardiology assessment
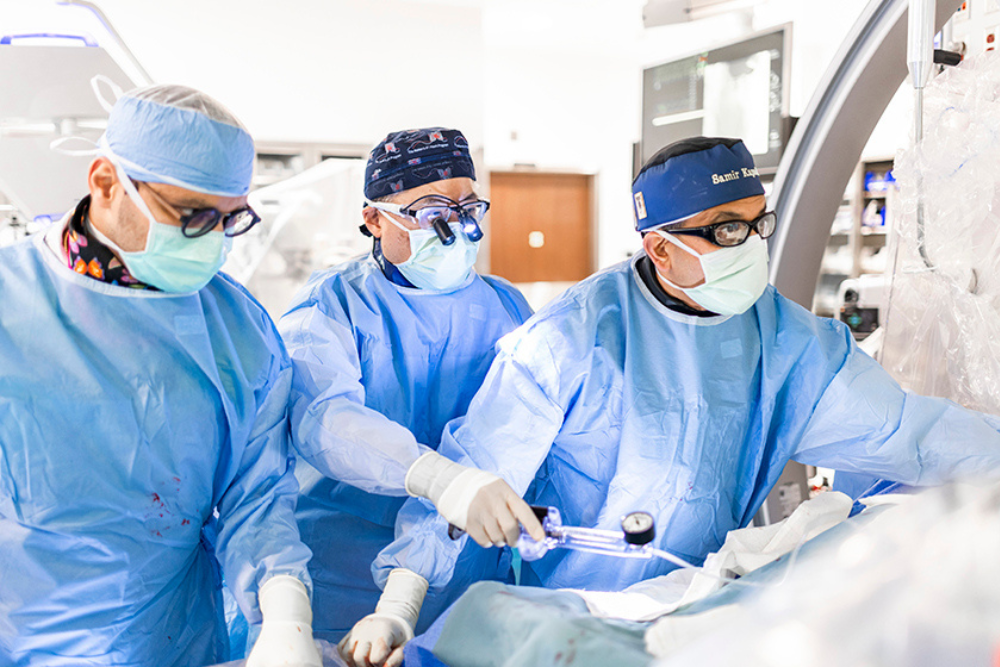
Delivering precise repair without open surgery
Interventional treatments include device closures for ASD, VSD, and PDA, balloon angioplasty or valvotomy for narrowed valves, and stenting for coarctation or vessel obstruction. These procedures use a thin catheter inserted through a blood vessel, minimizing discomfort and eliminating surgical incisions. Children recover quickly, often returning home within a day or two. Follow-up ensures the device remains stable, heart function improves, and complications are prevented, providing safer long-term outcomes.
FAQS
Your questions answered for safer decisions
Yes, it is very safe when performed by experienced pediatric interventional cardiologists using advanced imaging, precision devices, and strict safety protocols designed for children.
Most procedures take one to two hours, depending on defect size, complexity, and child’s anatomy, with monitoring afterward to ensure stable recovery.
Only a tiny puncture mark remains at the catheter entry site, avoiding large surgical scars and reducing discomfort significantly for children.
Most children resume normal activities within a week, although strenuous exercise should be avoided until the cardiologist confirms complete healing for safe and sustained recovery progress.
Yes, general anesthesia is typically used to keep children still, comfortable, and safe throughout the procedure for best results.
In most cases, closure devices and stents remain lifelong, though periodic monitoring ensures proper function and early detection of rare long-term issues.
